Journal of the American College of Cardiology’de yayımlanan bir makaleye göre, yaygın kullanılan bir antibiyotik sınıfı olan makrolidler ufak ancak ölçümlenebilir ani kardiyak sorunlara neden olabiliyor. Makrolidler pnömoni, bronşit ve cinsel yolla bulaşan bazı hastalıkların tedavi edilmesinde kullanılıyor. Araştırmada, 1966 ve 2015 arasında yapılan ve 20 milyondan fazla hastanın dahil olduğu 33 araştırma analiz edildi; makrolid veya diğer tür antibiyotik alan veya antibiyotik almayan hastalar karşılaştırıldı. Makrolidler arasında eritromisin, azitromisin, klaritromisin ve kinolon türü antibiyotikler yer alıyor.
Widely Used Antibiotics May Raise Heart Risks, Review Finds
Macrolides were linked to small, but significant, chances of sudden cardiac death
![]()
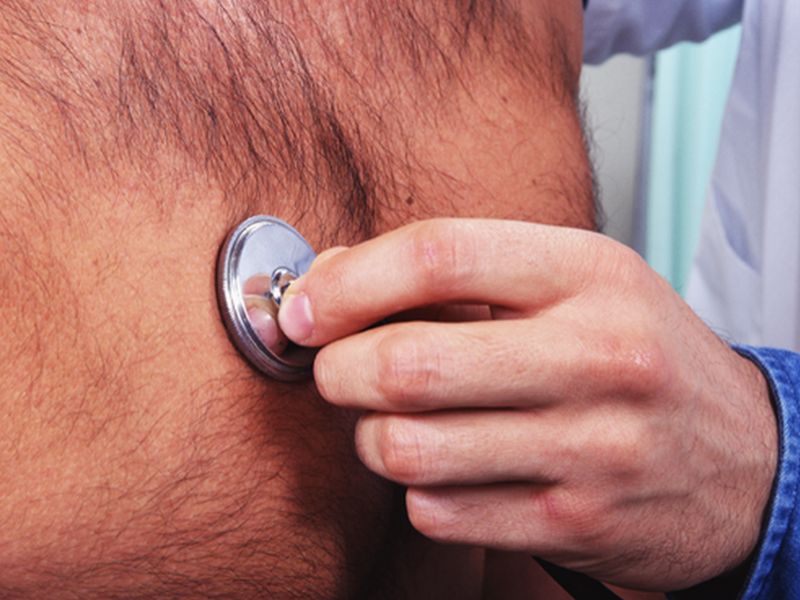
MONDAY, Nov. 9, 2015 (HealthDay News) — A widely used class of antibiotics is associated with a small but measurable increased risk of sudden cardiac death, researchers report.
These antibiotics — called macrolides — are used to treat infections such as pneumonia, bronchitis and some sexually transmitted diseases.
In the new report, the investigators analyzed 33 studies that were conducted between 1966 and 2015, and included a total of more than 20 million patients. The studies compared patients who took macrolides, other types of antibiotics, or no antibiotics.
Macrolides include the antibiotics erythromycin, azithromycin (Zithromax), clarithromycin (Biaxin) and quinolone.
The results revealed a small, but statistically significant, association between taking macrolides and increased risk of sudden cardiac death. But the review did not prove a cause-and-effect relationship between these medications and sudden cardiac death.
The study was published Nov. 9 in the Journal of the American College of Cardiology.
“The absolute risks of sudden cardiac death and cardiac death are small, so it should likely have limited effect on prescribing practice,” study author Dr. Su-Hua Wu, from the department of cardiology at First Affiliated Hospital at Sun Yat-Sen University in Guangzhou, China, said in a journal news release.
“However, given that macrolides are one of the most commonly used antibiotic groups, and millions of patients are prescribed these drugs annually, the total number of sudden cardiac deaths or ventricular tachyarrhythmias and cardiac deaths may not be negligible,” Wu added.
An average of 80 cases of rapid heartbeat that can result in sudden cardiac death (or “ventricular tachyarrhythmias”) occurred per 1 million treatment courses among patients who were not taking macrolides, the investigators found.
But, current use of macrolides was associated with an additional 118 ventricular tachyarrhythmias or related sudden cardiac deaths per 1 million treatment courses. And there were 36 additional sudden cardiac deaths from causes other than ventricular tachyarrhythmia, and 38 additional heart-related deaths per one million treatment courses, the findings showed.
Past use of macrolides and use of other antibiotics were not associated with increased heart risk, the researchers found.
To put the findings into perspective, one in 8,500 patients treated with macrolides could develop a serious heart rhythm problem and one in 30,000 might die, Dr. Sami Viskin, from the Tel Aviv Medical Center and Sackler School of Medicine at Tel Aviv University in Israel, explained in an accompanying journal editorial.
Viskin said macrolides are a first-line treatment for a number of infections.
“Today, when antimicrobial resistance represents a major threat to global health and new treatment options are frighteningly few, losing an entire class of antibiotics would represent a major setback in the fight against infections. Furthermore, it takes years to fully understand the consequences of a drug’s disappearance,” Viskin wrote.
More information
The U.S. Centers for Disease Control and Prevention has more about antibiotics.
SOURCE: Journal of the American College of Cardiology, news release, Nov. 9, 2015
— Robert Preidt
Last Updated:
Copyright © 2015 HealthDay. All rights reserved.