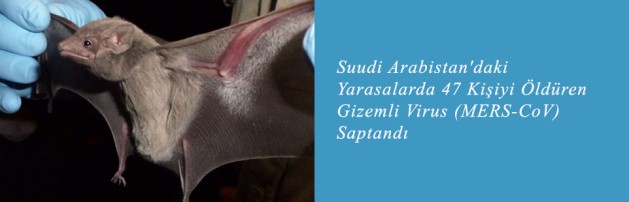
Mystery Virus That’s Killed 47 Is Tied to Bats in Saudi Arabia
By DONALD G. McNEIL Jr.
Published: August 21, 2013
WASHINGTON — Health officials confirmed Wednesday that bats in Saudi Arabia were the source of the mysterious virus that has sickened 96 people in the Middle East, killing 47 of them.
The outbreak of Middle East Respiratory Syndrome, or MERS, has been going on for 15 months, with most victims falling ill in Saudi Arabia and others growing sick after having traveled to the Middle East. In a study released Wednesday, an international team of doctors blamed coronavirus in bats for the human outbreak, but said that many questions remained, in part because a perfect match for the virus was found in only a single insect-eating bat out of about 100 Saudi bats tested. And since such bats do not normally bite people, drool on fruit or do other things that might transmit the disease to people, it was still unclear how the virus leapt to humans.
The bat is a Taphozous perforatus, or Egyptian tomb bat, which roosts in abandoned buildings, and the virus was found in a fecal sample.
So it is possible, said Dr. Jonathan H. Epstein, a veterinarian with the EcoHealth Alliance who helped trap the bats, that victims, like shepherds who might seek shelter in the buildings, picked it up by breathing in dried bat guano — similar to the way that Americans have been infected with hantavirus while sweeping up dried mouse droppings.
But it is also possible that an animal picked it up that way and then infected a human. Pigs, for instance, can get Nipah virus from bats and then pass it to humans in slaughterhouses.
Further tests on camels, sheep, goats and a cow will be finished soon, said Dr. W. Ian Lipkin, head of Columbia University’s Center for Infection and Immunity, which has already done 15,000 polymerase chain reaction tests tracking the virus.
“It’s a huge amount of work,” he said.
It has been known for several months that bats in Africa and Eastern Europe carried viruses related to MERS, but the relevant virus had not been found in Middle Eastern bats before. Camels in Oman have shown antibodies to a similar virus.
Knowing that one bat had an identical virus is a start, but more testing will be needed, said Dr. Ziad A. Memish, the Saudi deputy health minister who was a co-author on the study and gave a presentation on the virus in Washington on Wednesday.
The infected bat was in an abandoned house in a date palm orchard in Bisha, a small Saudi Arabian city. Investigators from Columbia and EcoHealth Alliance took samples there because the first known victim of the MERS outbreak was a businessman who had lived in Bisha and had his business, a large paint warehouse, nearby. The warehouse had a large garden with fruit trees and insects that attract many kinds of bats. The victim, a wealthy 60-year-old man, got sick in mid-June and died two weeks later, Dr. Lipkin said.
The victim also owned four pet camels that were sampled, but those results are not in yet, Dr. Lipkin added. Samples taken from livestock in countries with endemic foot-and-mouth disease must first be delivered to an Agriculture Department laboratory on Plum Island, Mass., to be certified negative for foot-and-mouth before they can be released for further testing.
Those restrictions can add months to the testing process, Dr. Memish said. That is one reason the bat samples were tested sooner, although other problems emerged: one of two frozen shipments of bat samples – the one the positive bat was in – was opened at Customs on entry into the United States and had thawed out by the time it reached Dr. Lipkin’s lab 48 hours later.
What was recovered from that sample, however, was a 100 percent match, which is virtually unheard of in virology, the study said.
The victim from Bisha had separate houses for his three wives and was building a fourth for a woman he planned to marry, “which suggests he was still vigorous,” Dr. Lipkin said.
But most of those killed by the new virus were old and had chronic conditions like diabetes or heart disease. Cases are being found of younger, healthier victims who often have milder symptoms, according to Dr. Memish, so it may soon be established that the disease’s mortality rate is much lower than 60 percent.
In his presentation Wednesday, hosted in Washington by the University of Pittsburgh Medical Center’s Center for Health Security, Dr. Memish said he only learned of the existence of the new virus in his own country when he read about it late last September on ProMED, an outbreak-alert service.
Dr. Memish said that by then, it was too late to advise travelers not to come to the annual pilgrimage to Mecca, which draws 4.5 million pilgrims. “That put an incredible strain on our system,” he said.
His department ordered all Saudi hospitals to look for and report unusual cases of pneumonia. The virus does not spread easily from person to person, but there have been case clusters in which family members or nurses and doctors who cared for patients were infected.
This year, the kingdom has suggested that older people, very young children and those in ill health or with suppressed immune systems not make the pilgrimage.