Antibiyotiklere dirençli bakteri
ABD’de bir kadın hastada tüm antibiyotiklere dirençli bakteri tespit edildi. ABD’li yetkililer, “Şimdiye kadar enfeksiyonlarla ilgili geliştirilen yöntemlerde yolun sonuna gelmiş olabiliriz” yorumunu yaptı.
ABD’nin Pensilvanya eyaletinde 49 yaşındaki bir kadında şimdiye kadar uygulanan tüm tedavilere olumsuz yanıt veren bir bakteri tespit edildi. Ülkede karşılaşılan antibiyotiğe dirençli ilk vakayla antibiyotiklerin etkisi konusundaki endişeler de yeniden gündeme geldi. Daha önce Çin ve Avrupa’da görülen vakalarda, bu bakteride antibiyotiğe dirençli mcr-1 isimli bir gen bulunmuştu. E.koli tipindeki bu bakterinin genetik değişikliklere uğrayarak şimdiye kadar etkili olan Colistin isimli antibiyotiğe yanıt vermediği açıklandı.
YOLUN SONU OLABİLİR
ABD Hastalıkları Kontrol ve Önleme Merkezi’nden Thomas Frieden, kadının idrar yolları enfeksiyonunda E.koli bakterisine rastlandığını ve bu tür enfeksiyonlarda kullanılan tüm antibiyotik tedavilerinin denendiğini belirterek, “Deneyebileceğimiz en eski antibiyotik olan Colistin’i de denedik ama kâbus bakterisi olarak adlandırabileceğim bu bakteri için işe yaramadı” dedi. Bakterinin “karbapenem dirençli enterobakterler” sınıfından olduğu belirtilirken, Amerikan Mikrobiyoloji Topluluğu’nun dergisinde de yayımlanan makalede, böyle bir vakaya ABD’de ilk kez rastlandığının altı çizilerek yetkililer önlem almaya çağrıldı. İsmi açıklanmayan kadının şimdiye dek yurtdışına çıkmadığını da vurgulayan Frieden, hastanın bakteriyi nereden almış olabileceğine ilişkin fikirleri olmadığını söyledi. Frieden, bu vakayla yeni bir antibiyotik dünyasına giriş yaptıklarını belirterek, şimdiye kadar enfeksiyonlarla ilgili geliştirilen yöntemlerde yolun sonuna gelmiş olmaktan korktuklarını dile getirdi.
Woman found to harbor infection resistant to antibiotic of last resort
The CDC says it’s working with health officials in Pennsylvania to determine how the patient may have contracted the bacteria.Video provided by Newsy Newslook
 Corrections and clarifications: An earlier version of this story misstated the extent of antibiotic resistance seen in a woman’s E. coli infection.
Corrections and clarifications: An earlier version of this story misstated the extent of antibiotic resistance seen in a woman’s E. coli infection.
For the first time, doctors have diagnosed an American with an infection that can’t be treated with an antibiotic of last resort, an ominous development in the battle against antibiotic resistance, according to a new study.
The antibiotic, colistin, is used when infections become impervious to all other drugs, including a class of antibiotics called carbapenems. Colistin, which was approved in the 1950s, fell out of favor in the 1970s because of its toxicity. Doctors have resumed using it when nothing else works.
In the past six months or so, scientists have found bacteria that are resistant to colistin in more than two dozen countries, said study co-author Patrick McGann, a senior microbiologist at the Walter Reed National Military Medical Center in Bethesda, Md. Given the danger of colistin-resistant bacteria, doctors at Walter Reed decided to begin testing samples from the U.S.
“People have begun looking for it,” McGann said. “And now that they’re looking for it, they’re finding it. It’s only a matter of time before these bacteria start showing up.”
The first patient with a colistin-resistant E. coli infection is a 49-year-old woman, who sought care for a urinary tract infection at a Pennsylvania clinic in April. Doctors sent her lab sample to the Walter Reed National Military Medical Center in Bethesda, Md., where researchers analyzed the bacteria’s genes.
The good news was that the woman’s infection was susceptible to a handful of antibiotics, including carbapenems, said study co-author Kurt Schaecher, service chief for the infectious disease lab at Walter Reed. That means her infection was treatable.
“We risk being in a post-antibiotic world,” said Thomas Frieden, director of theCenters for Disease Control and Prevention, who wasn’t involved in the new study, published Thursday in Antimicrobial Agents and Chemotherapy, published by the American Society of Microbiology. “The medicine cabinet is empty for some patients.”
Health officials have warned for years of the growing danger of antibiotic-resistant “nightmare bacteria,” which have evolved ways to avoid being killed by standard drugs. The problem is fueled by overuse of antibiotics, which are used not only in medicine but also food production.
One in three antibiotic prescriptions is unnecessary, the CDC announced last month. President Obama last year announced a National Action Plan for Combating Antibiotic-Resistant Bacteria to address the problem.
Although the problem is serious, the number of bacteria resistant to colistin is still relatively small in the U.S. and Europe, said Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota. McGann said the U.S. has a lower risk of superbugs than other countries, because doctors here prescribe antibiotics more prudently than in many places.
Antibiotics revolutionized medicine in the mid-20th century, making surgeries safer. If infections can’t be treated by antibiotics, people could die from small wounds or minor surgery. Already, about 700,000 people a year die from resistant infections, according to the Review on Antimicrobial Resistance, a project commissioned by the British government, in collaboration with the Wellcome Trust. In the U.S. alone, 2 million people develop resistant infections each year and 23,000 die, according to the CDC.
Bacteria today are mutating faster than pharmaceutical companies are developing drugs to kill them. Because most people take antibiotics for a few days or a week, they aren’t very profitable, giving drug companies little incentive to invest in them.
The last new class of antibiotics was discovered in 1984, according to a new report from the Pew Charitable Trusts.
“The major pharmaceutical companies have dropped many of their anti-infective programs over the last decade,” said Peter Hotez, director of the Sabin Vaccine Institute at Texas Children’s Hospital Center for Vaccine Development in Houston. “We’re going to need new actors to take on programs of antimicrobial resistance, including small and midsize biotechs, non-profit product development partners and developing country manufacturers.”
Two senators — Michael Bennet, D-Colo. and Orrin Hatch, R-Utah — have introduced legislation to speed up the approval of new antibiotics, called the Bennet-Hatch PATH Act. The bill would allow the Food and Drug Administration to expedite an antibiotic’s approval for an “identifiable, limited patient population,” such as those with antibiotic-resistant infections, if the drug treats a serious or life-threatening condition and addresses an unmet need.
“This is terrifying news,” Bennet said in a statement. “We need new drugs to fight these antibiotic-resistant bacteria that pose serious and unique challenges to health care professionals.”
The superbug that doctors have been dreading just reached the U.S.
For the first time, researchers have found a person in the United States carrying bacteria resistant to antibiotics of last resort, an alarming development that the top U.S. public health official says could mean “the end of the road” for antibiotics.
The antibiotic-resistant strain was found last month in the urine of a 49-year-old Pennsylvania woman. Defense Department researchers determined that she carried a strain of E. coli resistant to the antibiotic colistin, according to a study published Thursday in Antimicrobial Agents and Chemotherapy, a publication of the American Society for Microbiology. The authors wrote that the discovery “heralds the emergence of a truly pan-drug resistant bacteria.”
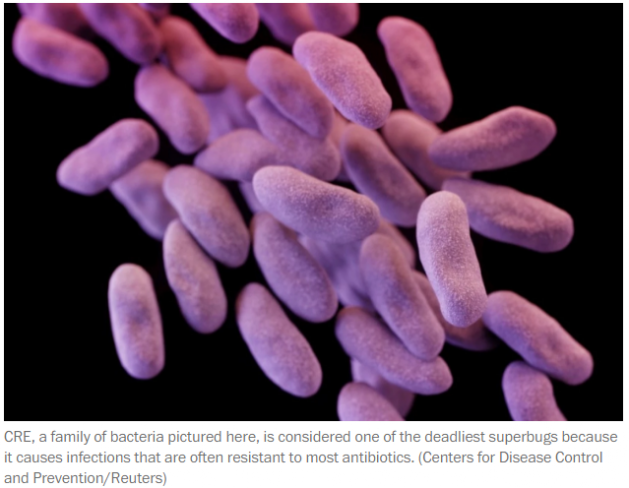
Colistin is the antibiotic of last resort for particularly dangerous types of superbugs, including a family of bacteria known as CRE, which health officials have dubbed “nightmare bacteria.” In some instances, these superbugs kill up to 50 percent of patients who become infected. The Centers for Disease Control and Prevention has called CRE among the country’s most urgent public health threats.
Health officials said the case in Pennsylvania, by itself, is not cause for panic. The strain found in the woman is still treatable with other antibiotics. But researchers worry that its colistin-resistance gene, known as mcr-1, could spread to other bacteria that can already evade other antibiotics.
It’s the first time this colistin-resistant strain has been found in a person in the United States. In November, public health officials worldwide reacted with alarm when Chinese and British researchers reported finding the colistin-resistant strain in pigs and raw pork and in a small number of people in China. The deadly strain was later discovered in Europe and elsewhere.
In this Nov. 2015 video, Centers for Disease Control and Prevention director Dr. Thomas Frieden said that the CDC is committed to fighting antibiotic resistance. (YouTube/CDC)
“It basically shows us that the end of the road isn’t very far away for antibiotics — that we may be in a situation where we have patients in our intensive care units, or patients getting urinary-tract infections for which we do not have antibiotics,” CDC Director Tom Frieden said in an interview Thursday.
“I’ve been there for TB patients. I’ve cared for patients for whom there are no drugs left. It is a feeling of such horror and helplessness,” Frieden added. “This is not where we need to be.”
Separately, researchers at the Agriculture Department and the Department of Health and Human Services reported that testing of hundreds of livestock and retail meats turned up the same colistin-resistant bacteria in a sample from a pig intestine in the United States. USDA said it is working to identify the farm the pig came from.
CDC officials are working with Pennsylvania health authorities to interview the patient and family to identify how she may have contracted the bacteria, including reviewing recent hospitalizations and other health-care exposures. The CDC hopes to screen the patient and her contacts to see if others might be carrying the organism. Local and state health departments also will be collecting cultures as part of the investigation.
The woman was treated in an outpatient military facility in Pennsylvania, according to a Defense Department blog post about the findings. Samples were sent to the Walter Reed National Military Medical Center for initial testing. Additional testing was done by a special Defense Department system that tracks multi-drug-resistant organisms.
Thursday’s study did not disclose further details about the Pennsylvania woman or the outcome of her case. The authors could not be reached for comment. A spokesman at the Pennsylvania Department of Health was not immediately available to comment on the case.
Pennsylvania Gov. Tom Wolfe (D) issued a statement saying his administration immediately began working with the CDC and the Defense Department to coordinate “an appropriate and collaborative” response.
“We are taking the emergence of this resistance gene very seriously,” he said, adding that authorities will take all necessary actions to prevent it from becoming a widespread problem with “potentially serious consequences.”
Sen. Robert P. Casey Jr. (D-Pa.) said he is concerned about the reports. In a statement, Casey said he supported legislation for and participated in hearings about antibiotic-resistant bacteria, which he said “present an urgent public health problem that we must focus on intensively.” He said he planned to get a full briefing on the case in the coming days.
Colistin is widely used in Chinese livestock, and this probably led bacteria to evolve and gain a resistance to the drug. The gene probably leaped from livestock to human microbes through food, said Yohei Doi, an infectious-disease doctor at the University of Pittsburgh who has studied the problem.
This animated video from 2013 from the Centers for Disease Control and Prevention highlights the key points and graphics of the “Antibiotic Threats in the United States” report. (YouTube/CDC)
“Food handlers may be at higher risk,” he said. In places like China, where live animal markets are often in close proximity to food stalls, it may be more likely for the bacteria to spread from animals to humans.
He and other experts in infectious diseases called for speedier action to curb the overuse of antibiotics in livestock worldwide.
“It’s hard to imagine worse for public health in the United States,” Lance Price, director of the Antibiotic Resistance Action Center and a George Washington University professor, said Thursday in a statement about the case. “We may soon be facing a world where CRE infections are untreatable.”
Scientists rang the alarm bells about the gene in November, but not enough attention was paid. “Now we find that this gene has made its way into pigs and people, and people in the U.S.,” Price said. “If our leaders were waiting to act until they could see the cliff’s edge — I hope this opens their eyes to the abyss that lies before us.”
Scientists and public health officials have long warned that if the resistant bacteria continue to spread, treatment options could be seriously limited. Routine operations could become deadly. Minor infections could become life-threatening crises. Pneumonia could be more and more difficult to treat.
Already, doctors had been forced to rely on colistin as a last-line defense against antibiotic-resistant bacteria. The drug is hardly ideal. It is more than half a century old and can seriously damage a patient’s kidneys. And yet, because doctors have run out of weapons to fight a growing number of infections that evade more-modern antibiotics, it has become a critical tool in fighting off some of the most tenacious infections.
Bacteria develop antibiotic resistance in two ways. Many acquire mutations in their own genomes that allow them to withstand antibiotics, although that ability can’t be shared with pathogens outside their own family.
Other bacteria rely on a shortcut: They get infected with something called a plasmid, a small piece of DNA, carrying a gene for antibiotic resistance. That makes resistance genes more dangerous because plasmids can make copies of themselves and transfer the genes they carry to other bugs within the same family as well as jump to other families of bacteria, which can then “catch” the resistance directly without having to develop it through evolution.
The colistin-resistant E. coli found in the Pennsylvania woman has this type of resistance gene.
Public health officials say they have been expecting this resistance gene to turn up in the United States.
“This is definitely alarming,” said David Hyun, a senior officer leading an antibiotic-resistance project at the Pew Charitable Trust. “The fact that we found it in the United States confirms our suspicions and adds urgency to actions we need to work on antibiotic stewardship and surveillance for this type of resistance.”
Late last year, as part of a broader budget deal, Congress agreed to give hundreds of millions of dollars to the federal agencies engaged in the battle against antibiotic-resistant bacteria.
The largest chunk of that money, more than $150 million, was slated to go to the CDC as part of an effort to build and strengthen capacity at state and local health departments to prevent and monitor superbug outbreaks.
Other funding went to the National Institutes of Health for research on combating antimicrobial resistance, as well as to an agency known as BARDA, which works on national preparedness for chemical and biological threats, including developing new therapies.
A dreaded superbug found for the first time in a U.S. woman
The case was detailed in a report by the U.S. Department of Defense on Thursday. Centers for Disease Control and Prevention Director Dr. Tom Frieden talked about the case at the National Press Club in Washington.
The woman went to a clinic in Pennsylvania, and a sample was forwarded to Walter Reed National Military Medical Center. Walter Reed found the bacteria in her urine. There is no indication of how the bacteria got into the woman’s system. She had not traveled outside the United States within the past five months.
The CDC and the Pennsylvania Department of Health mobilized immediately to investigate the case and to trace contacts the patient may have had to see whether the bacteria had spread.
The woman was treated and released and has no other medical problems related to the bacteria that we know of, according to Dr. Alex Kallen, a medical officer with the CDC.
The CDC said it is looking for other potential cases in the health care facility the patient visited.
The bacteria have been identified in other infections outside the United States. Doctors saw cases in Europe, Canada and China.
The U.S. Department of Agriculture also found one strain of Colistin-resistant E. coli in a single sample of a pig intestine, according to a statement from the Department of Health and Human Services. The USDA is trying to determine what farm the pig came from to see whether any other animals were impacted.
These two cases are what the CDC characterized as a “warning sign, more than a catastrophe,” according to Kallen.
The concern is that traits of this rare mutant Colistin-resistent E. coli could jump to other bacteria that respond only to Colistin, creating a potentially unstoppable superbug.
One report suggests that antibiotic-resistant infections can result in the deaths of half the patients who become infected.
Antibiotic resistance has become a growing problem in this country. The World Health Organization has warned that it is one of the biggest threats to global health today.
Frieden warned that although this is the first case in the United States, we should expect to see more such superbugs in the near future. Frieden, who often warns doctors against overuse of antibiotics, urged scientists to develop new drugs quickly.
Each year in the United States, at least 2 million people become infected with other kinds of bacteria that can’t be beaten with most antibiotics, and at least 23,000 people die each year as a result of those infections,according to the CDC.
“The medicine cabinet is empty for some patients,” Frieden said. “It is the end of the road unless we act urgently.”
CNN’s Elizabeth Cohen contributed to this report.